Doctors Propose New Diagnosis: ‘Unable to Pay for Prescriptions’
Doctors Propose New Diagnosis: ‘Unable to Pay for Prescriptions’
(Bloomberg) -- If you get struck by lightning or bitten by a pig, a physician can record that information with a code shorter than your phone number.
But if you can’t afford your bills, doctors and health plans have no consistent way to document that.
Now the biggest U.S. insurance company and the country’s most influential association of doctors want to create new ways to better capture information about patients’ social conditions. It’s part of a shift in the health-care industry to address aspects of people’s lives that influence their well-being beyond medical care, so-called social determinants of health.
“Having a standardized diagnosis allows for everyone in the system to understand that there’s an unmet social need,” said Sheila Shapiro, a senior vice president at UnitedHealthcare. The company, a unit of Minnetonka, Minnesota-based UnitedHealth Group Inc., announced the plan Tuesday with the American Medical Association.
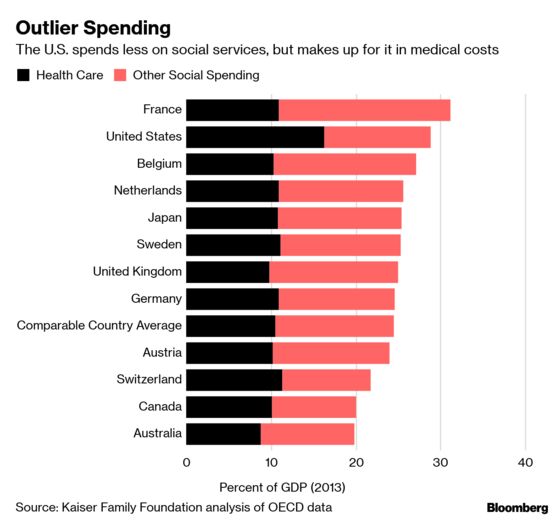
Medical care accounts for only about 20 percent of what determines a person’s health. The rest comprises behavior, social and economic factors, and environment. While the U.S. spends much more than peer countries on health care, it spends far less on a thinner social safety net.
Just as medical diagnoses trigger prescriptions or referrals to labs and specialists, the proposed codes are meant to help clinicians refer patients to assistance for food, housing, transportation or other needs.
Since 2017, UnitedHealthcare’s Medicare Advantage plans have made more than 700,000 referrals to outside social-service programs. The insurer’s Medicare plans cover about 4.9 million people.
Among the more than 20 new codes under consideration:
- unable to pay for prescriptions
- unable to afford child care
- worried about losing housing
- unable to count on family and friends
- feeling unsafe in current environment
Having standard designations for such conditions would let doctors, hospitals and health plans share the information through medical records and insurance claims forms.
“Everyone can start reading from the same sheet of music,” said Tom Gianulli, chief medical information officer at the AMA’s Integrated Health Model Initiative.
While the codes wouldn’t immediately lead to reimbursement changes, capturing data about patients’ social needs may be a step toward paying for interventions that address them.
“Collecting data is a big part of this right now, and trying to figure out what’s effective, and advocate for funding around that,” said Steve Nelson, chief executive officer of UnitedHealthcare.
Slowly Changing
Payments are still largely tied to the number of procedures clinicians perform, rather than the overall health of patients. That’s slowly changing, and the effort to treat social needs is part of the transformation.
For example, a diabetic who can’t get to the pharmacy to pick up medication may wind up in an emergency room with uncontrolled blood sugar. Traditionally, insurance would pay for the emergency room visit but not for the cab ride to the pharmacy that might have prevented it.
The taxpayers and employers who finance America’s $3.5 trillion medical system ultimately pay the cost of that hospital visit. The health-care industry and policy makers are struggling to figure out how to get people those cab rides, as well as other interventions that could make people healthier and reduce overall spending.
The industry has already taken steps in that direction. In 2016, the new codes were adopted to indicate whether a patient is homeless, poor or lacking adequate food, for example. The latest proposal would build on that effort. A federal committee will decide whether to adopt the proposal later this year.
New codes are a useful first step, but there are limits to what the health-care system can do, said Melinda Abrams, a vice president at the Commonwealth Fund, a foundation focused on health research.
Society also needs to properly finance the social-service system because inadequate funding contributes to high health-care costs, Abrams said.
“The health-care sector has had a blind eye to it.”
To contact the reporter on this story: John Tozzi in New York at jtozzi2@bloomberg.net
To contact the editors responsible for this story: Drew Armstrong at darmstrong17@bloomberg.net, Mark Schoifet, Timothy Annett
©2019 Bloomberg L.P.