(Bloomberg Opinion) -- The Covid-19 pandemic is meeting many of the worst expectations that public health experts in the U.S. and Europe had for fall and winter. There’s one thing they worried about that doesn’t seem to be happening, though: a devastating “twindemic” of Covid and seasonal influenza.
Instead, the flu is AWOL — so far at least. In New York City, which publishes a handy daily count of emergency-room visits for influenza-like illnesses and other conditions, numbers are running at less than one-third of the recent norm for the first half of December.
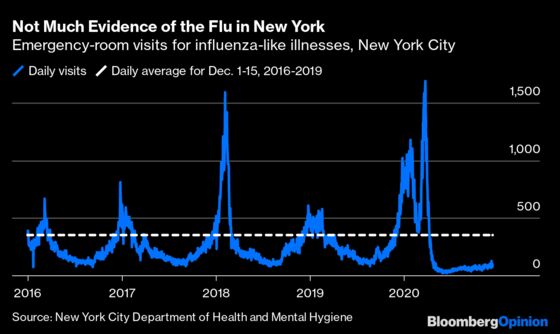
This seeming absence of influenza is almost certainly not just a lucky break. It’s also not the result of a coverup in which the authorities count flu cases as Covid-19 cases (apparently a popular theory in some Covid-denialist circles). It is conceivable that New York emergency rooms are less likely to count coronavirus cases as influenza-like illnesses than they were last March, when Covid tests were scarce and health-care workers less familiar with Covid symptoms. It’s also possible that people are just avoiding emergency rooms if they at all can. But positive influenza test results tracked on the U.S. Centers for Disease Control and Prevention’s FluView show an even more dramatic decline.
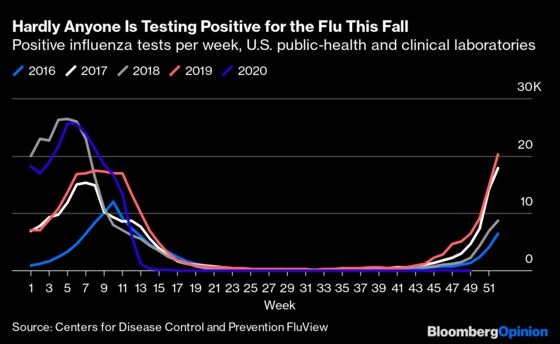
That dark-blue line that’s pretty much indistinguishable from zero for most of the year is 2020. The positive-test total for the week ending Dec. 5 — the most recent data available — was just 56. In the same week last year it was 6,435. The start of flu season in the northern hemisphere is generally deemed to be the 40th week of the year, which ended on Oct. 3, making Dec. 5 the end of the 49th week. Here’s a decade’s worth of positive-test totals for the first 10 weeks of flu season:
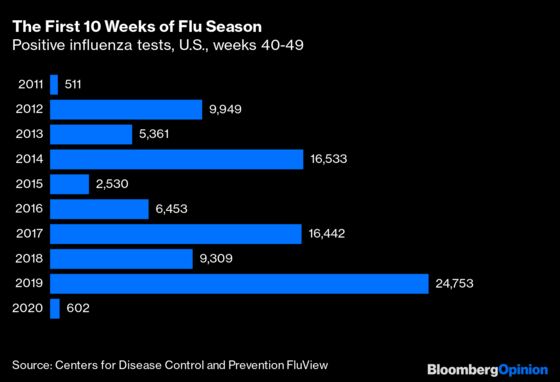
Yes, the 2011-2012 flu season started out with an even lower positive-test count. But that’s misleading, given that the number of flu tests performed has risen a lot since then (although it’s still nowhere near the number of Covid-19 tests performed this year). Those 511 positives in the first 10 weeks of the 2011-2012 flu season were out of 40,150 tests, for a positivity rate of 1.3%. This year’s 602 positives are out of 401,112 tests, for a positivity rate of 0.15%. By all appearances, then, this flu season in the U.S. is on track to be significantly milder than what turned out to be the least-deadly flu season of the past decade and possibly the least-deadly since the 1980s.
Similar trends are apparent all over the world. “In the temperate zone of the northern hemisphere, influenza activity remained below inter-seasonal levels,” the World Health Organization summed-up in its most recent weekly influenza update. That is, there’s less incidence of flu right now, in late fall, than there usually is in the summer. The WHO and other public-health agencies have been understandably hesitant to declare victory over the flu just yet — it’s still early in the season, and there’s another disease out there wreaking havoc even if the flu isn’t. The chief executive of smart-thermometer maker Kinsa Inc. is less reticent, telling the New York Times that “It looks like the twindemic isn’t going to happen.” And it’s clear from 2020 flu seasons that already ended that something out-of-the-ordinary is going on.
Studies have found that in the U.S. and Europe, flu incidence fell off much more sharply than usual in late winter and early spring this year. And in Australia, where peak flu season generally runs from April through September and Covid-control efforts were much more successful than in the U.S. or Europe, there was no flu season at all.
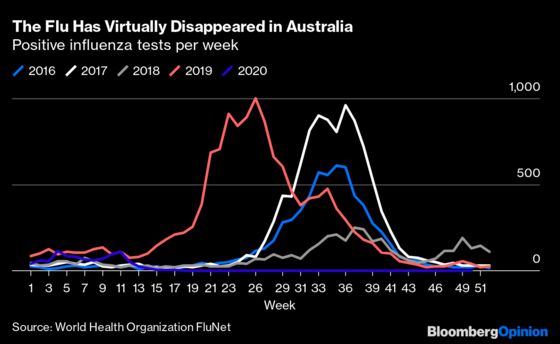
Since the beginning of May (the last full month of autumn in the southern hemisphere), five influenza tests have come back positive in Australia, according to the WHO’s FluNet database. Since the middle of July, none has. Other countries in the southern hemisphere’s temperate zones have had similar experiences.
Why is this happening? The push to get more people vaccinated against the flu this fall to avert the feared twindemic may have had some impact, but that doesn’t explain why flu incidence plummeted last spring. The obvious explanation is simply that the things that individuals and governments have been doing to slow the spread of Covid-19 have brought the spread of influenza, a respiratory disease that is transmitted in similar, if not identical fashion, to a screeching halt.
These measures have likely been more effective against influenza than against Covid because influenza is so much less contagious than Covid. A rough measure of contagiousness is the basic reproduction number — the number of people each person with the disease can be expected to infect if everyone behaves normally. For seasonal influenza it’s about 1.3, in flu pandemics it’s been higher than that but still below 2. For Covid-19 it’s probably somewhere between 2 and 4.
Mask-wearing, working from home, banning large gatherings and other social distancing measures — together with more people acquiring immunity by contracting Covid-19 — seem to have brought Covid’s effective reproduction number in the U.S. down to not much more than 1. (When last I checked the estimates on rt.live, Tennessee had the highest rate at 1.22 and Wyoming the lowest at 0.85.) By all appearances, that’s also pushed the effective reproduction number for the flu down well below 1.
One lesson from this is that the oft-heard lament that U.S. and many European countries have failed in battling the pandemic is wrong. Sure, a quick glance at East Asia makes clear that the West could have done much, much better. But given how successful we’ve been at halting the flu, it seems clear that we’ve also been successful at slowing down Covid. The resurgence of the disease this fall has been bad, but it could have been much, much worse.
Another lesson is that “non-pharmaceutical interventions,” the term of art for all the things we’ve been doing to slow Covid’s spread while waiting for vaccines, ought to be a bigger part of the toolkit for battling the flu. That’s not to say we should close all the borders and restaurants every winter, but lower-cost measures such as taking hand-washing seriously, wearing a mask when you don’t feel well, working from home if you’ve been exposed and keeping sick visitors and workers away from nursing homes could save thousands of lives every year. And if a new pandemic flu strain comes along that’s as deadly as, say, the 1918 variety (which was much deadlier than Covid-19, especially for young people), costlier interventions would almost certainly be worth the price.
The wait for a pandemic flu vaccine would be shorter than it has been for Covid-19. It took about six months from identification of a new strain of H1N1 influenza in 2009 to a vaccine being widely available. In a presentation last week at a European Scientific Working Group on Influenza conference, vaccinology professor Florian Krammer of the Icahn School of Medicine at Mount Sinai in New York said that with the right preparations, the wait could be shortened to three months. If mask mandates, social distancing and other non-pharmaceutical interventions can stop influenza, and it only needs to be stopped for three months, it would be crazy not to use them.
This column does not necessarily reflect the opinion of the editorial board or Bloomberg LP and its owners.
Justin Fox is a Bloomberg Opinion columnist covering business. He was the editorial director of Harvard Business Review and wrote for Time, Fortune and American Banker. He is the author of “The Myth of the Rational Market.”
©2020 Bloomberg L.P.