India Finds Itself At The Back of The Line For Virus Test Kits
Weeks into an outbreak that’s caused a national lockdown, India’s labs are largely standing idle.

(Bloomberg) --
As India races to head off the novel coronavirus pandemic, it’s empowered almost 200 state-run and private labs to conduct tests to determine who among its dense population has the virus.
Yet weeks into an outbreak that’s caused a national lockdown, those labs are largely standing idle. The 123 state-run labs are operating at only 36% capacity, while the 49 accredited private labs managed just an average of eight tests each on Monday, according to the Indian Council of Medical Research.
They say they lack test kits as India struggles to secure the foreign-made ones now in urgent demand globally. Meanwhile, red tape is slowing the deployment of locally made test kits.
“We don’t have kits at all,” said Nilesh Shah, the president of Metropolis Healthcare Ltd., one of the accredited private diagnostics firms, adding that government labs don’t have supplies either. “The priorities are going to countries where there is a major outbreak like Italy and Spain and the U.S. and the U.K. So all the major international vendors are saying I’m not sure how much I can allot for India.”
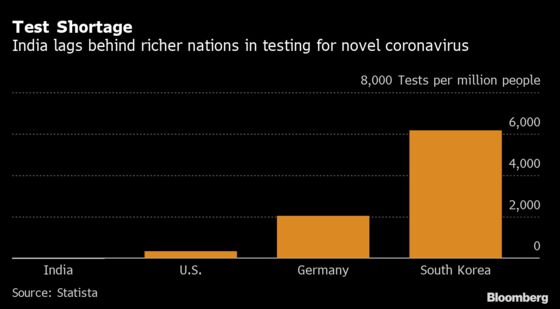
The number of tests in India stood at just 42,788 on March 31, one-thirtieth the pace of the U.S and even further behind that of top testing countries like South Korea.
The low rate has sparked speculation that India’s official tally of just under 2,000 infections is underestimating the true size of its outbreak as nations doing more testing report much higher case numbers. Densely packed cities and meager public finances make the country uniquely exposed to the kind of fast-moving contagion that’s overwhelmed health-care systems around the world.
While the danger of Covid-19 has prompted Prime Minister Narendra Modi to impose the world’s biggest lockdown, India has to compete with much richer countries for the chemicals used to assess a patient’s sample. While India has a vast manufacturing sector devoted to churning out generic drugs, its bio-pharmaceutical industry’s ability to make higher-end medication and devices -- like the virus test kits which identify the pathogen’s genetic sequence in a patient’s sample -- is still lacking.
The Indian Council for Medical Research referred questions on the impact of the testing kit shortage to the Ministry of Health and Family Welfare. A spokeswoman for the ministry didn’t respond to calls, emails and text messages requesting comment.
“Currently there is more demand than supply so everything is overpriced,” said Akoriaswamy Velumani, managing director of Thyrocare Technologies Ltd., another diagnostics company recruited for testing. “We buy test kits and sell the services. We don’t have adequate test kits, and adequate test kits are not available in the market.”

Can’t Get to Pune
With the bottleneck in foreign imports, pressure is growing for India to use locally-made kits. The government will accept kits already approved by the U.S. and European authorities, but local manufacturers need to go through a regulatory approval process which up to now has been conducted only by one government facility in the city of Pune, a three-hour drive from Mumbai.
With all trains, flights and railway services halted in the three-week lockdown, that means that any kit maker not based in Pune has not been able to get approval. Pune-based startup Mylab Discovery Solutions is the sole local maker approved at present and has the capacity to make 20,000 tests a day. It’s working to ramp that up, the company said in an emailed statement.
Others have been hampered. Trivitron Healthcare, a Chennai-based maker of medical devices, said it’s not been able to reach Pune but is hopeful that the planned addition of an evaluation center in Delhi, where Trivitron has its own office, may help it win approval for its own test kit as early as next week, said Managing Director G.S.K. Velu. Its test kit can produce results at a cost of 500 rupees ($6.50) per patient.
“Internationally it’s much more expensive,” he said. “The U.S. is paying much more. In India we have to innovate and bring it down to very low cost so people can actually afford it.”
©2020 Bloomberg L.P.