CVS Predicts an Ugly 2019 After Closing $68 Billion Aetna Deal
CVS Predicts an Ugly 2019 After Closing $68 Billion Aetna Deal
(Bloomberg) -- CVS Health Corp. said its results this year will be dragged down by rising costs and poor results from a 2015 takeover of nursing-home pharmacy Omnicare, raising questions about whether an ambitious $68 billion purchase of insurer Aetna last year was the right move for the health-care giant.
Just as it works to integrate one of the most ambitious deals in the health-care industry, CVS is being beset by bad news from all sides. A struggling nursing-home industry has created fewer customers for Omnicare, leading to $6.1 billion in writedowns. Higher wages and employee benefits cut into the gains from the 2017 corporate tax overhaul. And one of CVS’s main businesses, pharmacy-benefit management services for insurers and employers, is under attack in Washington.
On Wednesday, the Woonsocket, Rhode Island company said that adjusted earnings in 2019 will be $6.68 to $6.88 a share, compared with the $7.36 average of Wall Street estimates.
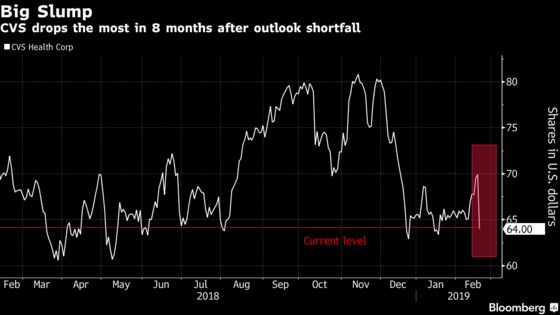
The shares fell as much as 9.4 percent, the worst intraday drop since June, when internet retail giant Amazon.com Inc. announced it was buying a pharmacy business that could compete with CVS.
Facing challenges to its business from all around, CVS on Wednesday dangled the possibility of cutting expenses to get profits back in line.
“We see additional opportunities to continue to manage our cost base and reduce our core to help mitigate those headwinds,” Chief Financial Officer Eva Boratto said on a call with analysts.
In a phone interview, Chief Executive Officer Larry Merlo said the main focus of new merged company is growth, not cost-cutting. He described the issues holding down profits at retail drugstores this year -- including a paucity of new generic drug introductions -- as transitory. And he said that CVS is committed to the nursing-home pharmacy arena despite the disappointing results so far.
“From my perspective, the two companies coming together are a growth story,” he said, referring to the Aetna deal. “You will see us continuing to invest in the business.”
The drugstore and pharmacy-benefits company’s future likely now depends on how its deal for health insurer Aetna turns out. CVS has said it will use the takeover, which closed in November, to create a vertically integrated health-care company that can better coordinate care and offer more services to customers.
But the Aetna deal may also come under more scrutiny from investors. The 2019 guidance was a “major disappointment,” said Evercore ISI analyst Ross Muken. It “will stoke fears the Aetna deal was defensive in nature.”
Until the Aetna takeover, CVS’s biggest deal in the last decade had been its acquisition of Omnicare, a pharmacy company that serves patients in nursing homes and long-term medical-care facilities. When the $12.9 billion deal was announced in 2015, CVS CEO Larry Merlo heralded it as creating new opportunities in a large and growing population of senior citizens.
Instead, those nursing-home customers have been going bankrupt amid declining occupancy rates and payment pressures, CVS said, leaving it with fewer customers to serve.
CVS announced a $2.2 billion writedown, following a $3.9 billion charge on the business in the second quarter. Together, they add up to almost half of what the company paid for Omnicare three years ago, and the unit is predicting more challenges in the future, CVS said.
The sector “has continued to experience industrywide challenges that have impacted our ability to grow the business at the rate that was originally estimated when the company acquired Omnicare,” CVS said.
Other Pressures
CVS also didn’t get as much of a benefit as it expected from the 2017 corporate tax law changes. While the corporate rate dropped from 35 percent to 21 percent, CVS had to give back some of those gains in the form of higher wages and benefits for workers.
In Washington, its pharmacy-benefits management business is under attack. The Trump administration has proposed significant changes to the system of rebates that drugmakers offer to CVS and other PBMs in return for covering their drugs.
The Trump administration’s proposed new rebate rule is “taking us backwards not forwards,” Merlo said on the conference call, and will lead to higher premiums for all seniors with Medicare drug plans. “It puts taxpayers on the hook and branded pharma ends up with a profit windfall.”
Critics have called the rebates a source of profits for PBMs, while CVS says it returns rebates to customers.
What Bloomberg Intelligence Says:“CVS’ 2019 guidance significantly below consensus makes it difficult to overcome the perception that its legacy retail and PBM units are facing long-term structural headwinds.”Jonathan Palmer, Health-Care Analyst Click here to read the research |
With the Aetna deal closure, CVS now has three main lines of business: retail drugstores and long-term care, health-care benefits, and pharmacy services. Despite the disappointing outlook for 2019, there were some bright spots in those businesses.
CVS’s pharmacies filled more prescriptions in the fourth quarter than a year prior, and front-of-store retail sales rose -- defying pressures from online sellers that have hurt the drugstore sector as a whole. Revenue and prescriptions in the pharmacy-benefits management segment rose as well.
To contact the reporter on this story: Robert Langreth in New York at rlangreth@bloomberg.net
To contact the editors responsible for this story: Drew Armstrong at darmstrong17@bloomberg.net, Cecile Daurat
©2019 Bloomberg L.P.