Insurers Figured Out How to Make a Profit in Obamacare Last Year
Insurers Figured Out How to Make a Profit in Obamacare Last Year
(Bloomberg) -- After years of losses, the U.S. health insurance industry figured out how make money from Obamacare last year, a new analysis shows.
The secret? Raising their prices.
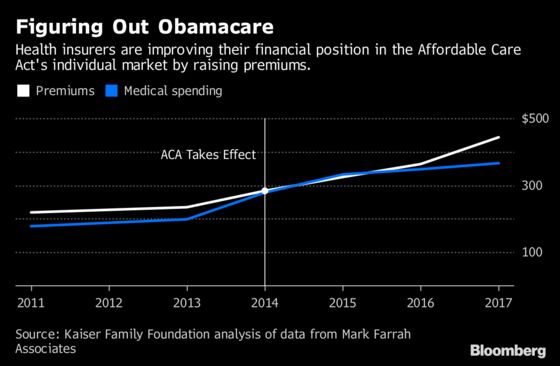
The average cost of health insurance plans sold in the individual market climbed about 22 percent in 2017, as insurers boosted premiums well above what they spent on medical care. That left many in a profitable position for the first time since the Affordable Care Act went into effect, according to a Kaiser Family Foundation report released Thursday.
Companies that have stuck with the program are facing fresh challenges. A law passed by Congress repealed the requirement that all people have health insurance, and the Trump administration has pushed to let companies offer health plans that don’t comply with the ACA’s rules.
To make up for those risks, some insurers are requesting big rate increases again for 2019.
“These new data from 2017 offer further evidence that insurers in the individual market are regaining profitability, even as political and policy uncertainty, repeal of the individual mandate penalty as part of tax reform legislation, and proposed regulations to expand loosely-regulated short-term insurance plans cloud expectations for the future,” according to the analysis.
Another big change not shown in the data: Insurers such as UnitedHealth Group Inc., Humana Inc. and Aetna Inc. that didn’t profitably sell Obamacare plans largely dropped out of the market by last year. That left behind the profitable insurers, but it also meant fewer health plan choices for people in many parts of the country.
Rising premiums have helped insurers’ bottom lines. They’ve also become a major pain point for consumers, and a rallying cry for opposition to the health law. While about 9.8 million people in the individual market get subsidies that insulate them from the rising cost of coverage, about 8 million others, mainly those with higher incomes, don’t get help. Some of those people have opted against buying insurance at all.
To contact the reporter on this story: Zachary Tracer in New York at ztracer1@bloomberg.net
To contact the editors responsible for this story: Drew Armstrong at darmstrong17@bloomberg.net, Timothy Annett
©2018 Bloomberg L.P.